- How can we help?
- +1 800-320-0230
- 225-927-8917
- info@bayoustatelab.com
Material Showdown: Zirconia vs E.max vs PFM vs Full Metal When to Choose What

Why The Right Lab Partner Changes Everything
September 22, 2025
Why Chair-side Time Is Your Most Valuable Asset And How the Right Lab Partner Helps You Save It
October 7, 2025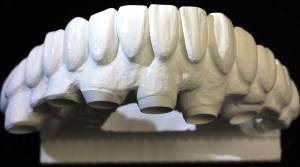
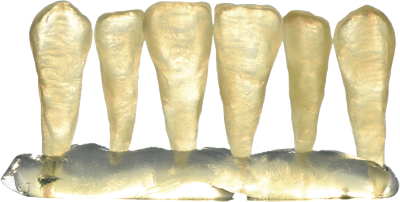
Material Showdown: Zirconia vs e.max vs PFM vs Full Metal When to Choose What
Because choosing the right restorative material isn't one-size-fits-all.
Between rapid advances in digital dentistry, evolving patient expectations, and an ever-expanding menu of restorative options, selecting the right crown material has never been more important< or more confusing. Should you choose zirconia for its brute strength? e.max for its beauty? Stick with reliable PFM for bridges? Or lean on time-tested full metal when clearance is tight? At Bayou State Crown & Bridge Lab, we see the results of these decisions every day. A well-chosen material can mean flawless margins, a smooth seat, and a happy patient. A poor choice can lead to remakes, chairside grinding, and unpredictable esthetics. Below, we break down the strengths, weaknesses, prep requirements, and ideal indications for the four most common fixed restorative materials we fabricate daily.
Zirconia: The Posterior Powerhouse
Best for:
- Posterior single units and bridges
- Bruxers and high-load occlusion
- Situations with limited reduction
- Full-arch frameworks and implant restorations
Why dentists choose zirconia:
- Superior strength (900–1200 MPa for monolithic zirconia)
- Excellent marginal integrity with digital workflows
- Less occlusal reduction needed compared to glass ceramics
- Polished zirconia is gentle on opposing enamel when finished correctly
- Newer multilayer esthetic zirconias offer improved translucency
Clinical considerations:
- Prep design: Chamfer or light shoulder margin, 0.8–1.2 mm occlusal clearance
- Avoid knife-edge preps with ragged margins — these can scan poorly and compromise fit
- Maintain smooth, rounded line angles to avoid internal stresses and seating issues
- Pre-polished zirconia is more wear-friendly than glazed surfaces long term
Esthetics:
- Modern multilayer zirconias offer good shade blending, but they still lack the glass-like depth of lithium disilicate. For highly esthetic anterior work, zirconia can be layered with porcelain, but that introduces chipping risk.
Lab communication tips:
- Note desired shade gradient (e.g., A2 incisal transition to A3 cervical) for multilayer blocks
- Indicate if you prefer stain & glaze or high polish finish
- Send bite scans and clear opposing to help with occlusal morphology
Zirconia shines when strength, reliability, and quick seating are top priorities.
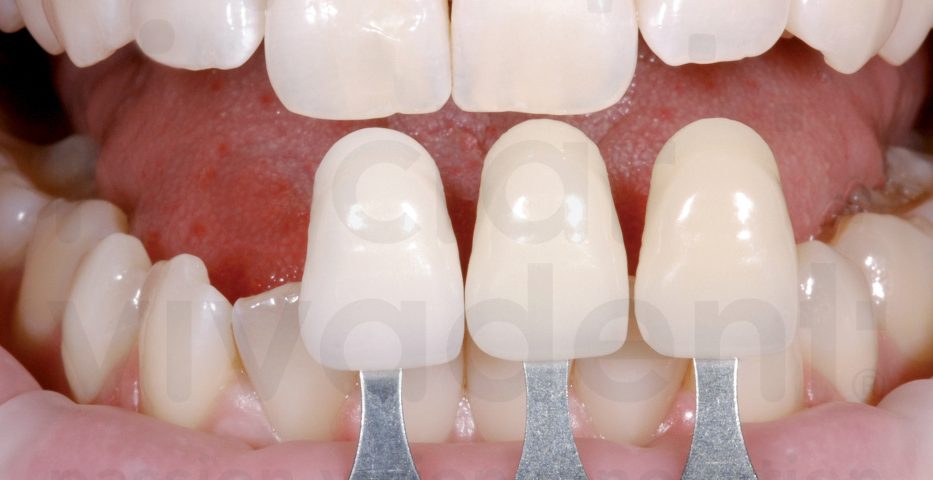
Lithium Disilicate: Esthetics Meets Strength
Best for:
- Anterior crowns and veneers
- Premolars where esthetics matter
- Conservative preps where bonding is planned
- Smile design and minimally invasive cases
Why dentists love it:
- Natural translucency that mimics enamel beautifully
- Bondable for thin restorations (e.g., veneers, onlays)
- Adequate strength (400–500 MPa) for most single-unit restorations
- Excellent marginal accuracy when prepped properly
Clinical considerations:
- Prep design: Rounded shoulder or deep chamfer, 1.5–2 mm occlusal, 1–1.5 mm axial
- Margins must be smooth and well defined—rough or beveled margins lead to thin, weak edges
- Stump shade matters: especially for thin veneers. Dark preps require an opaquer or high-value block
- Bonding is essential—resin cement with proper etch and silane is critical for strength
Esthetics:
- Lithium disilicate can achieve unmatched incisal translucency, surface texture, and light behavior. It is especially ideal for anterior esthetic zones where patients scrutinize shade and shape.
Lab communication tips:
- Always include stump shade, prep photos, and desired final shade
- Note if you plan to bond or cement—this affects block selection and thickness
- If using minimal prep veneers, communicate thickness targets clearly
e.max is your go-to for anterior beauty and conservative restorative approaches.
PFM: The Reliable Hybrid
Best for:
- Multi-unit bridges (especially posterior)
- Situations needing metal strength + porcelain esthetics
- Functional load areas
- Angled abutments or limited restorative space
Why dentists still use PFM:
- Decades of clinical reliability
- Excellent strength from metal substructure
- Customizable esthetics with layered porcelain
- Adaptable to many prep styles and clinical situations
Clinical considerations:
- Buccal reduction: 1.5–2 mm to support porcelain
- Lingual reduction: 1–1.2 mm for metal
- Margins: Shoulder with rounded internal line angles for porcelain; chamfer for lingual collar
- Be cautious of unsupported porcelain at porcelain–metal junctions — a classic chipping risk
- Consider lingual metal collars for strength and longevity on molars
Esthetics:
- PFMs can achieve beautiful results in skilled hands but may show a metal collar or gray substructure at gingival margins, especially with thin tissue. Ideal for posterior bridges or when metal strength is needed.
Lab communication tips:
- Specify collar design (none, thin metal, or porcelain butt)
- Indicate desired metal shade (standard, gold-hue, opaque)
- Provide clear opposing to allow proper porcelain thickness for strength
PFMs remain a smart, versatile choice for bridges and functionally demanding situations.
Full Metal: The Unsung Hero
Best for:
- Second molars and posterior teeth with minimal clearance
- Bruxers and heavy occlusion cases
- Long-term functional restorations
- Patients prioritizing function and durability over esthetics
Why dentists rely on full metal:
- Longest clinical track record of all materials
- Minimal reduction required, conserving tooth structure
- No porcelain to chip or delaminate
- Excellent fit, marginal integrity, and longevity
Clinical considerations:
- Prep design: 0.8–1 mm functional occlusal reduction, 0.5–0.8 mm non-functional
- Chamfer or feather-edge margins acceptable
- Smooth continuous margins are critical for a perfect lab fit
- Ideal for tight interocclusal spaces where other materials can't meet minimum thickness
Esthetics:
- Obviously limited—but in second molar positions, this is rarely an issue.
Lab communication tips:
- Indicate if you prefer yellow gold-hue or standard alloy for esthetics
- Confirm occlusal anatomy preferences (anatomic vs simplified for bruxers)
- Provide accurate bite registration—metal restorations typically have zero give
Full metal is the most forgiving, longest-lasting, and cost-effective option when esthetics are secondary.
Quick Comparison Table:
|
Zirconia |
900-1200 |
Posterior crowns, bruxers, full arches |
Smooth margins, avoid sharp angles; polish > glaze for wear |
|
|
e.max |
400-500 |
|
Anterior crowns, veneers, premolars |
Proper bonding & stump shade critical |
|
PFM |
High(metal) |
|
Bridges, complex cases, functional load |
Porcelain fracture risk at junction; collar design matters |
|
Full Metal |
Highest |
|
Molars, bruxers, limited space |
Esthetics limited but clinically unmatched for longevity |
Let's Plan Your Next Case Together
At Bayou State, our certified technicians are trained to evaluate these factors and recommend the ideal restorative pathway for each case. Whether you're restoring a single molar, designing a smile makeover, or planning a full-arch rehab, we'll help you pick the right material from the start.
We are a family-owned, faith-led, nationally certified dental laboratory with 40 years experience. We specialize in cosmetic makeovers, implant restorations, custom abutments, and digital workflows, proudly supporting dentists across Louisiana and beyond